HANOVER, N.H. – Sept. 25, 2020 – While declines in U.S. hospital admissions during the onset of COVID-19 has been well-documented, little is known about how admissions during the rebound varied by age, insurance coverage and socioeconomic groups. The decline in non-COVID-19 admissions was similar across all demographic subgroups but the partial rebound that followed shows that non-COVID-19 admissions for residents from Hispanic neighborhoods was significantly lower than for other groups. The findings are reported in a new study in Health Affairs(released as a Fast Track Ahead of Print article) conducted by a research team from Sound Physicians, Dartmouth College, and the Dartmouth Institute for Health Policy and Clinical Practice at the Geisel School of Medicine at Dartmouth.
Image 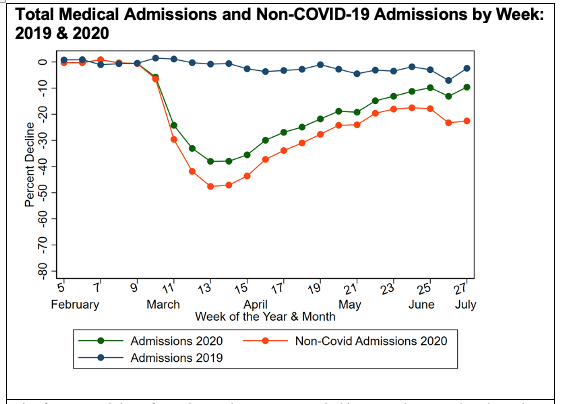 |
| This figure is Exhibit 1 from the study. Image provided by co-authors. Updated graph through early September available upon request from jon.skinner@dartmouth.edu. |
“Our study shows that patients from Hispanic neighborhoods did not have the same rebound in non-COVID-19 admissions as other groups, which points to a much broader issue of healthcare access and equity for lower-income and minority patients,” said senior author and health economist Jonathan Skinner, a professor at the Dartmouth Institute for Health Policy and Clinical Practice at the Geisel School of Medicine, and the James O. Freedman Presidential Professor in Economics at Dartmouth. As a result, these barriers may have contributed to higher in-hospital mortality rates in April for this group than for others,” he added.
The study drew on data from 1 million hospital admissions (from hospital administrative data and electronic medical and billing records) from Sound Physicians, a large nationally distributed medical group with hospitals throughout the U.S. The data came from 201 hospitals in 36 states, including areas hit hard early on by the pandemic, including Wash., Mich., Ohio, and the greater metropolitan area of New York.
The research team looked at non-COVID-19 admissions for the top 20 acute medical conditions, from early February through early July. They found that non-COVID-19 admissions fell in March and reached its lowest point in April. The rebound leveled off in June/July, which was when there was a resurgence of COVID-19 cases in some regions.
The study’s results reports the following:
- From February to April 2020, declines in non-COVID-19 admissions were similar across all demographic subgroups exceeding 20 percent for all primary admission diagnoses.
- The lowest point in non-COVID-19 admissions was in April during which the overall decline was 43 percent.
- By late June/early July 2020, non-COVID-19 admissions had only made a partial rebound at 16 percent below pre-pandemic baseline volume. (Updated data suggests this partial rebound continued through the summer.)
- During the June/July rebound period, non-COVID-19 admissions were substantially lower for patients from majority-Hispanic neighborhoods (32 percent below baseline) and remained well below baseline for patients with pneumonia (44 percent below baseline), chronic obstructive pulmonary disease/asthma (40 percent below baseline), sepsis (25 percent below baseline), urinary tract infection (24 percent below baseline) and acute ST-elevation myocardial infarction/heart attack (22 percent below baseline).
These particular diseases are reported in the results, as these were the acute conditions for which the declines were the highest. Most of the majority-Hispanic neighborhoods in this dataset were located in the Southwest and South— Calif., Ariz., Texas, and Fla.
The research team speculate that the declines in medical admissions may have been due in part to a fear of contracting COVID-19 by both physicians and patients, greater use of telemedicine, and possibly lower transmission rates of non-COVID-19 diseases following stay-at-home orders.
Available for comment are: Jonathan Skinner (jon.skinner@dartmouth.edu), senior author, and John Birkmeyer (jbirkmeyer@soundphysicians.com), lead author and chief clinical officer of Sound Physicians, and an adjunct professor at Dartmouth Institute for Health Policy and Clinical Practice at the Geisel School of Medicine at Dartmouth.
The study was co-authored by Amber Barnato and Nancy Birkmeyer at the Dartmouth Institute for Health Policy and Clinical Practice at the Geisel School of Medicine at Dartmouth, and Robert Bessler from Sound Physicians. The study was funded by the National Institute on Aging.

